XYLAZINE
Common Drug Names: tranq, tranq dope, zombie drug
Xylazine, a non-opioid veterinary tranquilizer not approved for human use, is a central nervous system depressant.
Xylazine is often added to illicit opioids, including fentanyl, and people report using xylazine-containing fentanyl to lengthen its euphoric effects. Most overdose deaths linked to both xylazine and fentanyl also involved additional substances, including cocaine, heroin, benzodiazepines, alcohol, gabapentin, methadone, and prescription opioids.
Taking opioids in combination with xylazine and other central nervous system depressants—like alcohol or benzodiazepines—increases the risk of life-threatening overdose. People report using xylazine or xylazine-containing drugs by injecting, snorting, swallowing, or inhaling. Xylazine is a central nervous system depressant that can cause;
- drowsiness
- amnesia
- slow breathing and heart rate
- dangerously low blood pressure
- skin ulcers
- abscesses
- other related complications
At very high doses, or with other central nervous system depressants, xylazine can cause:
- Loss of physical sensation
- Loss of consciousness
- Intensification of the effects of other drugs, which can complicate overdose presentation and treatment.
Overdosing from Xylazine:
Experts recommend giving the opioid overdose reversal medication naloxone because xylazine is frequently combined with opioids. However, because xylazine is not an opioid, naloxone does not address the impact of xylazine on breathing. Because of this, experts are concerned that a growing prevalence of xylazine in the illicit opioid supply may be less effective for some overdoses. Emergency medical services should always be alerted to a suspected overdose.
Withdrawal from xylazine is not a well-defined syndrome due to its "not approved for use in human" nature. However, it is reported to be more intense than opioid withdrawal, and there are far fewer options available to treat it. Symptoms of withdrawal include extreme anxiety that can last for months.
Opioid withdrawal symptoms can be treated with medications like methadone and buprenorphine, but xylazine withdrawal symptoms cannot be treated with these medications.
As the prevalence of xylazine has increased in the unregulated drug supply, there have been subsequent increases in the number of hospitalizations for skin wounds associated with substance use. Xylazine can cause skin wounds that are not associated with environmental factors (such as living unhoused and/or lacking access to hygiene facilities), but rather with use of the substance itself. These complex wounds often occur at skin sites associated with injection, but they can occur at skin sites that are not associated with injection and in individuals who don’t inject substances. Early intervention in treating xylazine-related skin wounds can prevent them from progressing into severe necrotic skin ulcerations. (Office of Addiction Services and Supports)
SAMHSA's National Helpline - 1-800-662-HELP (4357)
SAMHSA’s National Helpline is a free, confidential, 24/7, 365-day-a-year treatment referral and information service (in English and Spanish) for individuals and families facing mental and/or substance use disorders.
SAMHSA's Behavioral Health Treatment Services Locator
Narcotics Anonymous
Narcotics Anonymous offers recovery from the effects of addiction through working a twelve-step program, including regular attendance at group meetings. The group atmosphere provides help from peers and offers an ongoing support network for addicts who wish to pursue and maintain a drug-free lifestyle. Find an NA meeting near you.
For Providers: Minnesota Alliance of Rural Addiction Treatment Programs
Many places that distribute Fentanyl test strips also have strips that test for Xylazine;
To access fentanyl test strips, contact:
DRUG TRENDS
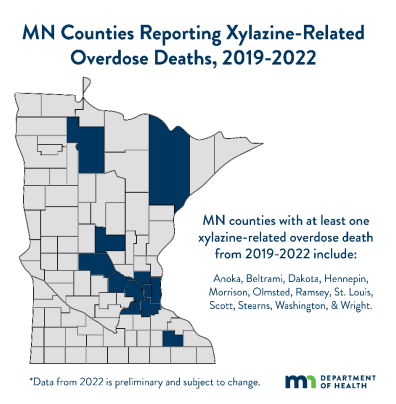
Xylazine-involved overdose deaths in Minnesota are relatively low compared to some states, but they are increasing at an alarming rate. The first known xylazine-involved overdose death in Minnesota occurred in 2019. Since then, the number of xylazine-involved deaths has increased every year. In 2019, there were four overdose deaths involving xylazine, followed by eight in 2022 and 24 in 2021.
Preliminary 2022 data shows there were 34 xylazine-involved deaths across the state. Minnesota counties with at least
one xylazine-related death from 2019-2022 include: Anoka, Beltrami, Dakota, Hennepin, Morrison, Olmstead, Ramsey, St. Louis, Scott, Stearns, Washington, and Wright.